A “mini heart attack” is a health emergency, and you must consult a doctor immediately to get the best medical assistance. Using the most advanced diagnostic methods and tests for detecting heart disease, Dr. Steven Reisman will focus on your symptoms and come up with the most effective solutions to help you live a better quality of life with improved heart health. He will evaluate your risk factors and schedule a health screening to identify if you have any blockages or heart disease and start with treatment immediately to prevent any further problems that could be life-threatening.
A “mini heart attack” feels like a heart attack with mild to severe chest pain, discomfort, and shortness of breath, but it only occurs for two to three minutes and then stops with rest. On the other hand, a full heart attack with complete blockage lasts much longer, sometimes even more than 20 minutes, and can be fatal in some cases.
Also called a mild heart attack or a non-ST elevation myocardial infarction (NSTEMI), a mini heart attack occurs when there is a temporary blockage in the coronary arteries. The symptoms experienced during a mini heart attack lack the intensity typically seen with a classic heart attack, and the heart may only suffer minimal damage as there is a partial blockage of the artery. This lack of intensity and the fact that an individual may feel normal during and after a “mini heart attack” are two reasons it is described as mild.
Symptoms like pain, pressure, tightness, or discomfort in the chest and other parts of the body such as arms, backs, or stomach are commonly reported during a heart attack. Research shows that there are several types of heart attacks and the mild heart attack may be a warning sign of a larger heart attack in the future.
Mini Heart Attack Symptoms
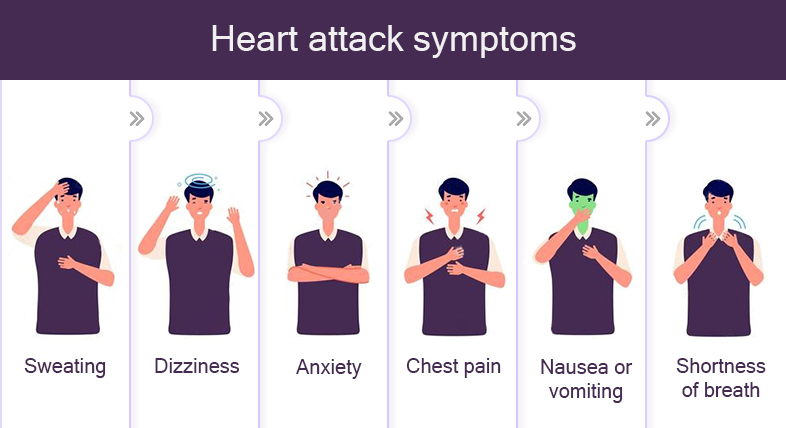
Symptoms of a “mini heart attack” are similar to a regular heart attack but they only last for a short time. They include:
- Chest pain or feeling of pressure or squeezing in the center of the chest that may last several minutes or comes and goes;
- Pain in the throat which is often confused with indigestion or heartburn;
- Fatigue;
- Belching or burping;
- Shortness of breath either before or during the discomfort and chest pain;
- Feelings of discomfort in the upper back, jaw, neck, and upper extremities;
- Pain or discomfort in the stomach;
- Feelings of lightheadedness or nausea;
- Breaking out into a cold sweat.
Women may also experience the following additional symptoms:
- Upper abdominal pain;
- Extreme fatigue or weakness.
These are worrying symptoms and must not be ignored or taken lightly. Seek immediate medical support if you experience any or all of these symptoms. Even if you are not sure it is a “mini heart attack”, it is best to consult a doctor to be certain and have your condition diagnosed by an expert.
What Causes Mini Heart Attacks?
A “mini heart attack” occurs when the arteries that supply blood to the heart become blocked and the part of the heart that normally gets blood from that artery is jeopardized. This blockage usually occurs due to a condition called coronary heart disease or coronary artery disease.
In coronary heart disease, the blood flow is affected by the blockage in the arteries caused by plaque that consists of fat, cholesterol, and other substances. Our heart needs oxygen-rich blood to function. The longer the heart does not get oxygen-rich blood, the more damage can occur.
Sometimes plaque also breaks free and causes blood clots that can block off the artery and prevent blood from reaching parts of heart muscles, leading to a heart attack. A “mini heart attack” often goes unnoticed but it can still cause some heart damage.
A silent heart attack can be as damaging as a classic one. Knowing the risks of a silent heart attack can help motivate you to begin a program of prevention.
Risk factors for coronary heart disease include:
- High blood pressure;
- Heredity;
- Diabetes;
- Smoking;
- Poor diet;
- Inactive lifestyle;
- Overweight/obesity;
- Stress.
Do not let these risk factors affect your health and life. Schedule an appointment with an expert heart doctor to know more about your condition and how you can reduce the possibility of a heart attack in the future.
Preventing a Heart Attack
Doctors recommend preventing a heart attack with a few lifestyle changes and managing the risk factors.
Lifestyle changes that can improve heart health include:
- Regular exercise;
- Maintaining a healthy weight;
- Monitoring your low-density lipoprotein (LDL) cholesterol levels;
- Changing diet according to your health and heart conditions;
- Stopping tobacco usage;
- Eating a more balanced diet comprising of lefty green vegetables and fresh fruits;
- Monitoring your sodium, sugar, and saturated fat intake;
- Increasing your intake of heart-healthy foods such as whole grains, walnuts, fatty fish;
- Managing stress with yoga and meditation.
Making positive changes in your lifestyle is the most effective way to reduce the risk of developing heart disease. As you manage your lifestyle and risk factors, the heart doctor will monitor your progress and help you achieve better heart health.
If you have already suffered from a heart attack or are at high risk of developing coronary artery disease, make sure to contact an experienced and qualified cardiac specialist close to you. Dr. Steven Reisman is a leading cardiologist at the New York Cardiac Diagnostic Center, a premier cardiovascular care facility with the most advanced diagnostic equipment for heart screening. He will examine you thoroughly and take your medical history to evaluate your heart condition and see what you have been going through. With the most beneficial solutions and treatment options, he will address any cardiac issues you may have to put your mind at ease and prevent any critical heart-related conditions in the long run.

Dr. Steven Reisman is an internationally recognized cardiologist and heart specialist. He is a member of the American College of Cardiology, American Heart Association, and a founding member of the American Society of Nuclear Cardiology.
Dr. Reisman has presented original research findings for the early detection of "high risk" heart disease and severe coronary artery disease at the annual meetings of both the American College of Cardiology and the American Heart Association. Dr. Reisman was part of a group of doctors with the Food and Drug Administration who evaluated the dipyridamole thallium testing technique before the FDA approved it.
Dr. Steven Reisman's academic appointments include Assistant Professor of Medicine at the University of California and Assistant Professor at SUNY. Hospital appointments include the Director of Nuclear Cardiology at the Long Island College Hospital.



